Benefits of biomarker testing
Biomarker testing is an essential tool in medicine, especially for cancer surveillance1. In the context of breast cancer, a variety of biomarkers provide important information about how the illness progresses and how well treatments work. Biomarker testing, alongside other monitoring methods, can provide benefits to healthcare professionals by offering specific patient care, more affordable testing, and improved patient comfort – all of which can contribute to enhanced patient outcomes2.
Biomarker testing can reduce healthcare costs
One of the greatest benefits of biomarker testing in breast cancer monitoring is the potential for reduced healthcare costs – both for healthcare providers and patients – without compromising overall treatment quality. This is achieved through an increasing accessibility in testing and the effectiveness of testing, which can guide clinicians to reducing the use of unnecessary treatments.
Biomarker testing accessibility is on the rise
The cost of cancer treatment and biomarker testing varies based on the test type, cancer type, and insurance coverage3. In the United States, Medicare and Medicaid cover some tests for advanced cancer, while private insurance may cover tests that are proven necessary for treatment decisions and have clinical utility4. In Europe, coverage depends on country, disease, and accessibility, with higher rates of adoption and access in countries with public national reimbursement processes5.
As technology advances and methodologies refine, biomarker testing has become more accessible globally. With this increased accessibility, it has become more affordable for patients and healthcare providers. In a retrospective investigation in Canada from April 2010 to March 2013, the frequency of biomarker testing for lung cancer increased from 46% in the initial year to 60% in the final year for EGFR (epidermal growth factor receptor) testing and from 5% to 40% for ALK (anaplastic lymphoma kinase) testing6. This affordability allows healthcare providers to offer comprehensive testing to a broader patient population.
Mitigating unnecessary treatments with biomarker testing
In oncology, biomarker testing can inform treatment decisions by recognizing specific genetic mutations or protein expressions that render tumors susceptible to targeted therapies2. Clinicians can optimize therapeutic outcomes by selecting treatments based on biomarker profiles rather than employing a one-size-fits-all approach while minimizing adverse effects and treatment-related expenses.
The strategic use of biomarker testing therefore has the potential to mitigate unnecessary treatments and interventions, which can lead to substantial cost savings across the healthcare system. By precisely identifying biomarkers indicative of disease presence, progression, or response to therapy, clinicians can tailor treatment plans to individual patients and avoid the administration of therapies that may yield limited benefits or pose unnecessary risks.
A case study from Biovica
A health economics study was conducted to estimate the diagnostic and treatment budget impact of the DiviTum® TKa assay—a blood-based biomarker test that measures Thymidine Kinase activity in the bloodstream—on the use for monitoring of HR+ postmenopausal metastatic breast cancer (MBC) patients undergoing treatment in a one-million-member U.S. health plan. Studies have shown that an increase in TK1 expression is linked to proliferating and aggressive cancer types7. The test is developed to monitor and predict treatment response in hormone receptor-positive postmenopausal MBC patients.
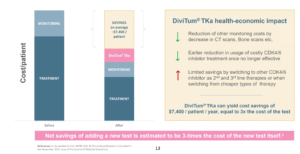
The budget impact model compares the inclusion and exclusion of DiviTum TKa to standard care under which DiviTum TKa:
1. reduces the frequency of traditional mBC monitoring tools
2. predicts treatment futility in advance of radiological disease progression.
Traditional disease monitoring assessment schedules were based on guidelines and expert opinions. DiviTum TKa’s impact on therapy utilization was based on published literature and expert opinion. Modeled costs
included DiviTum TKa, NCCN-recommended treatments, imaging, biomarker testing, and adverse events. A calculated total cost of per-member per-month (PMPM) with a 3-year time horizon8.
The findings showed expected savings of approximately 3x the spend on the DiviTum TKa test. Results were most sensitive to the DiviTum TKa cost, population parameters, and treatment costs8.
The clinical use of the DiviTum TKa assay is expected to decrease traditional imaging and monitoring. It may reduce the overall cost of managing metastatic MBC if it leads to clinical decisions to avoid futile therapy. Post-coverage, real-world monitoring of palliative therapies in the post-menopausal MBC patient population is needed to categorize cost savings over time better8.
Potential for early detection and intervention of cancer
Additionally, biomarker testing facilitates the early detection of diseases2, which can allow for timely interventions to prevent or hinder disease progression and reduce the need for more costly and intensive treatments in later stages. By identifying biomarkers associated with disease susceptibility or early-stage pathology, clinicians can implement preventive measures or initiate treatment interventions when diseases are most responsive to therapy, thereby averting the costly interventions required at advanced disease stages.
A case study from CVS Health
A study funded by CVS Health examined the total cost of care for patients with non-small cell lung cancer receiving broad versus restricted panel biomarker testing. An average of $1,200 US was added to the initial costs of broad panel testing. However, because of increased treatment efficacy, patients who underwent broad panel testing had monthly savings of almost $8,500 US per member9. There is, however, a scarcity of articles where the cost of breast cancer treatment has been precisely measured and stated.
In essence, the strategic utilization of biomarker testing enhances patient care as it optimizes treatment selection and improves outcomes. It also contributes to significant cost savings within the healthcare system by reducing unnecessary treatments and enabling early intervention strategies.
Biomarker testing can reduce patient discomfort while providing added-value data
Blood-based biomarker testing has the potential to reduce patient discomfort. Unlike traditional diagnostic procedures like biopsy, histology, or mammography, which may involve invasive techniques or discomfort, blood-based biomarker testing requires a simple, relatively painless, and non-invasive blood draw10. This ease of collection makes biomarker testing more accessible and acceptable to patients when integrated into routine check-ups, and it can reduce anxiety and potentially improve overall satisfaction with the healthcare experience.
Furthermore, integrating breast cancer biomarker testing alongside other screening and monitoring methods can enhance the comprehensive assessment of disease progression2. For instance, by combining biomarker data with imaging studies, clinical assessments, and other diagnostic modalities, healthcare providers gain a more intricate understanding of the patient’s condition. This holistic approach allows for earlier detection of disease recurrence or progression, which can enable timely interventions and personalized treatment strategies.
In oncology, blood-based biomarkers can complement imaging studies such as CT scans or MRIs that provide additional insights into tumor dynamics and breast cancer treatment response. By monitoring biomarker levels over time, clinicians can detect subtle changes indicative of disease progression or treatment resistance11.
Overall, the comfort and convenience offered by biomarker testing, mainly through non-invasive blood-based methods, empower patients to engage in their healthcare while actively minimizing discomfort and inconvenience. Additionally, the integration of biomarker testing into comprehensive monitoring protocols enhances the accuracy and timeliness of disease assessment, which ultimately results in improved outcomes and better quality of life for patients.
Biomarker testing can enhance patient outcomes
Cancer drugs work through various mechanisms, and biomarker testing has enhanced researchers and clinicians’ understanding of the disease, as certain biomarkers play key roles in disease development and behavior monitoring. Biomarker tests have been able to help healthcare providers determine the effectiveness of specific drugs against particular cancers and for particular patients11.
A Norwegian case study
Advancements in health, particularly in cancer treatment, are often attributed to progress in biomarker technology. Biomarker tests have significantly enhanced our understanding of the disease by helping identify which drugs are more effective against certain cancer kinds with certain mutations.
A study conducted in Norway12 aimed to assess whether the development of biomarker testing to guide cancer treatment and the availability of several cancer drugs has improved health outcomes. The assessment focused on premature mortality (potential years of life lost before the age of 75 or 65) and 3-year survival rates among cancer patients.
The analysis utilized patient-level data from the Cancer Registry of Norway, supplemented by drug sales data from the Norwegian Drug Wholesales Statistics. The Cancer Registry provided detailed information on each patient, which includes date of diagnosis, age at diagnosis, gender, cancer type, and stage at diagnosis. Data on cancer drugs and their indicated cancer types were obtained from the Thériaque drug database using WHO ICD-10 codes.
Two samples were used for the analysis: one focusing on premature mortality and the other on 3-year survival rates. Patients under 30 or over 75 years old, as well as those diagnosed with multiple cancers, were excluded from the research. Drug sales data were used as a proxy for drug utilization, and drugs requiring biomarker testing were identified using information from the FDA website and PharmGKB. These patients were monitored from 2000 to 2016, taking into recording the mortality caused by cancer within the period.
Due to the synergy between biomarker testing and the availability of cancer drugs, the analysis revealed a positive effect on the improvement in health outcomes. Biomarker-guided therapies were said to be associated with a significant decrease in premature mortality. This could be attributed to the personalization of treatment following the identification of cancer molecular specificities from the result of biomarker testing.
The study ends with the suggestion that biomarker testing and guided therapies hold promise in reducing premature mortality. However, further research is needed to understand better the long-term effects of biomarker-guided therapies on specific cancer treatment outcomes13.
As biomarker tests are becoming a vital component of the clinical management of cancers and other diseases, it is pertinent that healthcare providers understand the options available to them.
Biomarker testing can enhance disease treatment
Molecular classifications of breast cancer (BC) offer valuable insights for prognosis and guiding treatment strategies. Assessing hormone receptor (HR) status, particularly estrogen receptor (ER) and progesterone receptor (PR), has become a standardized approach to identify patients suitable for endocrine therapies such as selective ER modulators (SERM), aromatase inhibitors (AIs), as well as anthracycline and taxane-based chemotherapy14.
Furthermore, human epidermal growth factor receptor 2 (HER2) status is commonly assessed in BC biopsies to inform treatment decisions, which include the use of monoclonal antibodies (mAbs), antibody-drug conjugates (ADCs), tyrosine kinase inhibitors (TKI), poly ADP-ribose polymerase (PARP) inhibitors, and cyclin-dependent kinase (CDK) 4/6 inhibitors15.
As initially stated, biomarkers such as estrogen receptor (ER), HER1 & HER2, and others are essential in guiding treatment plans for individual patients. For instance, patients with ER-positive breast cancer benefit from hormone-targeted therapies like tamoxifen and toremifene, which block the estrogen receptor and inhibit tumor growth. Similarly, HER2-positive breast cancer patients can receive targeted therapies like trastuzumab, pertuzumab, and ado-trastuzumab emtansine (T-DM1), which specifically target HER2-positive cells16.
This approach, known as precision medicine, can enhance treatment efficacy and minimizes adverse effects, thereby improving patient tolerance and quality of life during the treatment journey.
Additionally, studies using biomarkers encourage the investigation of novel therapeutic approaches, such as immunotherapies and targeted medication combinations, that are specific to the molecular features of certain malignancies. Biomarker testing enables doctors to provide more effective and customized medicines by clarifying the molecular landscape of breast cancer and discovering actionable targets. This eventually improves patient outcomes and changes the therapeutic landscape for breast cancer.
A promising future for personalized medicine
Biomarker testing can significantly benefit patients and healthcare providers in disease monitoring and research when used in the appropriate contexts and alongside other testing and screening methods. Their unique ability to provide valuable insights into disease progression and treatment efficacy paves the way to a future where patients can receive more personalized – and potentially more effective – solutions. If you are interested in procuring the test for your clinic or research, you can contact us for more information.
References
- Seale, Katelyn N. and Katherine H R Tkaczuk. “Circulating Biomarkers in Breast Cancer.” Clinical Breast Cancer. Vol. 22, 3, pp. e319-e331. 3 April 2022. https://www.sciencedirect.com/science/article/pii/S1526820921002640
- Das, Sreyashi, et. al. “Biomarkers in Cancer Detection, Diagnosis, and Prognosis.” Sensors. Vol. 24 (1), 37. Published online 23 December 2023. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10780704/
- “Biomarker Tests and Cancer Treatment.” American Cancer Society. https://www.cancer.org/cancer/diagnosis-staging/tests/biomarker-tests.html
- “Improving Access to Biomarker Testing: Advancing Precision Medicine in Cancer Care.” American Cancer Society: Cancer Action Network. September 2020. https://www.fightcancer.org/sites/default/files/Improving%20Access%20to%20Biomarker%20Testing_FINAL.pdf
- Normanno, Nicola, et. al. “Access and quality of biomarker testing for precision oncology in Europe.” European Journal of Cancer. Vol. 176, pp. 70-77. November 2022. https://www.sciencedirect.com/science/article/pii/S0959804922005305
- Lim, C., et al. “Biomarker Testing and Time to Treatment Decision in Patients with Advanced Nonsmall-Cell Lung Cancer.” Annals of Oncology. Vol. 26, 7, 2015, pp. 1415–1421. https://pubmed.ncbi.nlm.nih.gov/25922063/
- Bitter, E. E., et al. “Thymidine kinase 1 through the ages: a comprehensive review.” Cell & Bioscience. Vol. 10, 138. Published 27 November 2020. https://cellandbioscience.biomedcentral.com/articles/10.1186/s13578-020-00493-1
- Carlson, J.J. et. Al ” Budget impact analysis of the DiviTum TKa assay in postmenopausal women with hormone receptor positive metastatic breast cancer.” Journal of Medical Economics, 24(1), 1309–1317. https://doi.org/10.1080/13696998.2021.2003674
- Brito, Rogelio Alberto, et al. “Total Cost of Lung Cancer Care Associated with Broad Panel versus Narrow Panel Sequencing.” Journal of Clinical Oncology: Official Journal of the American Society of Clinical Oncology. Vol. 38, no. 15_suppl, 2020, pp. 7077–7077. doi:10.1200/jco.2020.38.15_suppl.7077.
- Li, Jiawei, et al. “Non-Invasive Biomarkers for Early Detection of Breast Cancer.” Cancers. Vol. 12, no. 10, 2020, p. 2767. Published 27 September 2020. https://pubmed.ncbi.nlm.nih.gov/32992445/
- Afzal, Samia, et. al. “Breast Cancer; Discovery of Novel Diagnostic Biomarkers, Drug Resistance, and Therapeutic Implications.” Front Mol Biosci. Vol. 9: 783450. Published online 21 February 2022. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8899313/
- D′Avó Luís, Ana Beatriz, and Mikyung Kelly Seo. “Has the development of cancer biomarkers to guide treatment improved health outcomes?” The European Journal of Health Economics. Vol. 22 (5), pp. 789-810. Published online 30 March 2021. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8214594/
- Kittaneh, Muaiad, et al. “Molecular Profiling for Breast Cancer: A Comprehensive Review.” Biomarkers in Cancer. Vol. 5, 2013, p. BIC.S9455. https://journals.sagepub.com/doi/10.4137/BIC.S9455
- Parise, Carol A., et al. “Breast Cancer Subtypes as Defined by the Estrogen Receptor (ER), Progesterone Receptor (PR), and the Human Epidermal Growth Factor Receptor 2 (HER2) among Women with Invasive Breast Cancer in California, 1999-2004.” The Breast Journal. Vol. 15, no. 6, 2009, pp. 593–602. https://pubmed.ncbi.nlm.nih.gov/19764994/
- Pernas, Sonia, and Sara M. Tolaney. “HER2-Positive Breast Cancer: New Therapeutic Frontiers and Overcoming Resistance.” Therapeutic Advances in Medical Oncology. Vol. 11, 2019, p. 175883591983351. https://pubmed.ncbi.nlm.nih.gov/30911337/
- Schick, Jason, et al. “Breast Cancer Therapeutics and Biomarkers: Past, Present, and Future Approaches.” Breast Cancer: Basic and Clinical Research. Vol. 15, 2021, p. 117822342199585. https://pubmed.ncbi.nlm.nih.gov/33994789/